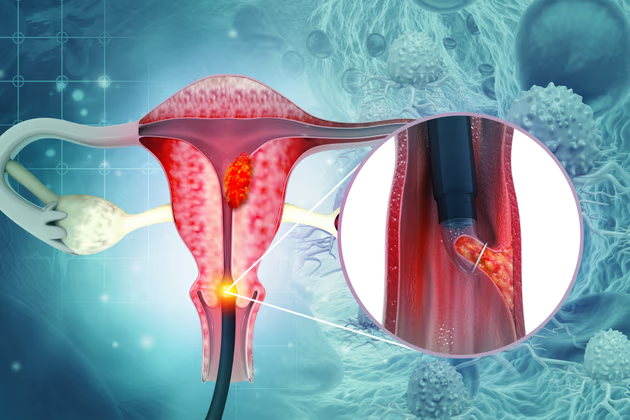
Cervical Cancer
Cervical cancer is a type of cancer that develops in the cervix — the lower part of the uterus that connects to the vagina. It is one of the most preventable and treatable forms of cancer when detected early through regular screening and vaccination.
With increased awareness, early diagnosis, and advanced medical treatments, the survival rate of cervical cancer has improved significantly.
What is Cervical Cancer?
Cervical cancer occurs when abnormal cells in the cervix grow uncontrollably. Most cases are caused by persistent infection with high-risk types of Human Papillomavirus (HPV), a common sexually transmitted virus.
Cervical cancer usually develops slowly over time. Before cancer forms, the cervical cells go through precancerous changes called cervical dysplasia, which can be detected through screening tests.
Causes of Cervical Cancer
The primary cause of cervical cancer is long-term infection with high-risk HPV strains, especially HPV-16 and HPV-18.
Other Risk Factors Include:
- Early sexual activity
- Multiple sexual partners
- Weak immune system
- Smoking
- Long-term use of oral contraceptives
- Lack of regular Pap smear screening
- Family history of cervical cancer
HPV infection is common, but most infections clear naturally. Persistent infection increases cancer risk.
Symptoms of Cervical Cancer
Early-stage cervical cancer often does not cause noticeable symptoms. As the cancer progresses, symptoms may include:
- Abnormal vaginal bleeding (between periods, after intercourse, or after menopause)
- Unusual vaginal discharge (watery, pink, or foul-smelling)
- Pelvic pain
- Pain during intercourse
- Heavier or longer menstrual periods
Advanced cervical cancer may cause:
- Back pain
- Leg swelling
- Difficulty urinating or bowel problems
- Fatigue and weight loss
Any abnormal bleeding should be evaluated by a healthcare provider immediately.
Types of Cervical Cancer
There are two main types:
- Squamous Cell Carcinoma: The most common type, arising from the outer lining of the cervix.
- Adenocarcinoma: Develops from glandular cells in the cervical canal.
In rare cases, mixed types can occur.
Stages of Cervical Cancer
Cervical cancer is classified into stages based on the size and spread of the tumor:
- Stage I: Cancer confined to the cervix.
- Stage II: Spread beyond the cervix but not to the pelvic wall.
- Stage III: Spread to the lower vagina or pelvic wall.
- Stage IV: Spread to nearby organs (bladder, rectum) or distant organs.
Early-stage cervical cancer has a high cure rate with appropriate treatment.
Diagnosis of Cervical Cancer
Regular screening plays a crucial role in early detection.
- Pap Smear Test: Detects abnormal or precancerous cervical cells.
- HPV Test: Identifies high-risk HPV strains.
- Colposcopy: A detailed examination of the cervix using a special microscope.
- Biopsy: A tissue sample confirms the diagnosis.
- Imaging Tests: CT scan, MRI, or PET scan may be used to determine cancer spread.
Treatment Options for Cervical Cancer
Treatment depends on the stage, tumor size, and overall health of the patient.
- Surgery: Removal of abnormal tissue (early stage), hysterectomy (removal of uterus and cervix), or radical hysterectomy for advanced cases
- Radiation Therapy: Uses high-energy beams to destroy cancer cells.
- Chemotherapy: Drugs used to kill or shrink cancer cells, often combined with radiation.
- Targeted Therapy & Immunotherapy: Advanced treatments that focus on specific cancer cells or boost immune response.
Early-stage cervical cancer can often be cured with surgery alone.
Prevention of Cervical Cancer
Cervical cancer is highly preventable with proper measures:
- HPV Vaccination: The HPV vaccine protects against high-risk HPV strains and is recommended for girls and boys starting at age 9–14.
- Regular Screening: Women should undergo routine Pap smears and HPV tests as recommended by their healthcare provider.
- Safe Sexual Practices: Using protection and limiting sexual partners reduces HPV risk.
- Quit Smoking: Smoking weakens the immune system and increases cancer risk.
Cervical Cancer Screening Guidelines
- Women aged 21–29: Pap smear every 3 years.
- Women aged 30–65: Pap smear + HPV test every 5 years (or Pap test alone every 3 years).
- After 65: Screening may stop if prior results were normal.
Consult your doctor for personalized screening recommendations.
Living with Cervical Cancer
A diagnosis can be emotionally challenging. Support systems are important for recovery and mental well-being.
Patients are encouraged to:
- Follow treatment plans carefully
- Maintain a balanced diet
- Stay physically active as advised
- Seek counseling or support groups
- Attend regular follow-up appointments
Early detection significantly improves survival rates and quality of life.
When to See a Doctor?
Seek medical advice if you experience:
- Unusual vaginal bleeding
- Persistent pelvic pain
- Abnormal discharge
- Pain during intercourse
Do not ignore symptoms — early evaluation saves lives.
